 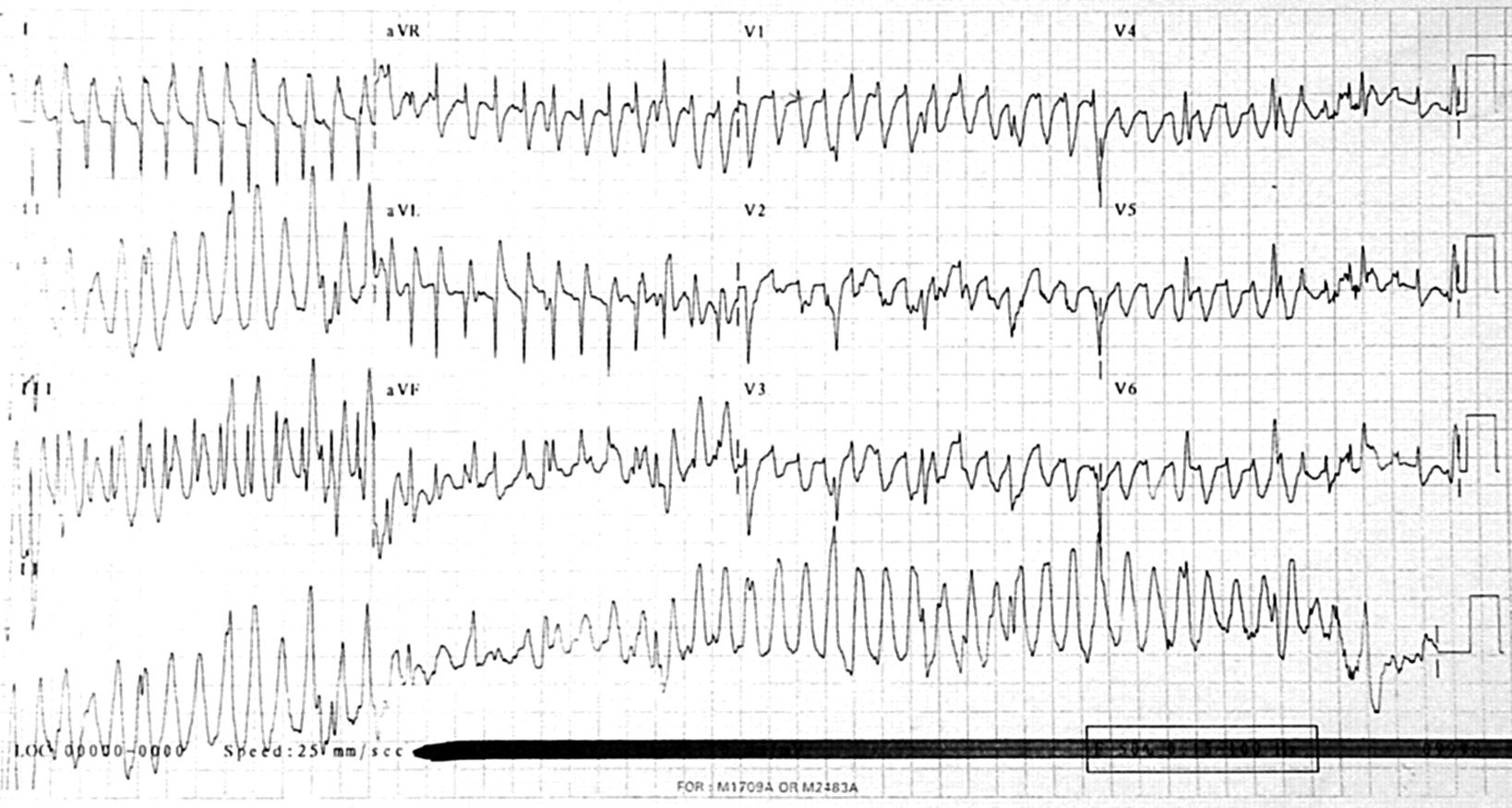
In this context, the fundamental question is whether rhythm analysis improves CPR delivery compared to the standard treatment, that is, cycles of 2 minutes of uninterrupted CPR followed by a hands-off interval for rhythm assessment. This does not reflect the real application scenario in which the objective would be to continuously analyze the rhythm during CPR. The current evaluation standard is based on the sensitivity and specificity of a single analysis using short duration (10–20 s) segments. In addition, the impact these methods would have on CPR delivery is unknown. As Li and Tang phrased it back in 2009, performance is good but not enough. However, the specificity rarely exceeds 85%, well below the 95% AHA goal. Most studies report sensitivities above 90%, the minimum value recommended by the AHA for AED performance. Strategies have focused either on adaptive filters to suppress the CPR artifact or, more recently, on approaches based on the direct analysis of the corrupted ECG. Over the last 15 years, many efforts have been made to reliably analyze the rhythm during CPR. Therefore, reliable rhythm analysis methods during chest compressions would be of great value. In fact, a recent multicenter study found an 18% decrease in survival to hospital discharge for every 5 s increase in preshock pause length. These interruptions, known as hands-off intervals, adversely affect the probability of restoration of spontaneous circulation (ROSC) after the delivery of the shock and compromise circulation. Interruptions for rhythm analysis alone take between 5.2 s and 28.4 s in commercial AEDs. The mechanical activity from the chest compressions introduces artifacts in the ECG that substantially lower the capacity of an AED’s shock advice algorithm (SAA) to detect shockable (sensitivity) and nonshockable (specificity) rhythms. However, CPR must be interrupted for a reliable AED rhythm analysis. Consequently, current resuscitation guidelines emphasize the importance of high-quality CPR with minimal interruptions in chest compressions. 
Over the years, evidence has accumulated suggesting that minimizing the interruptions in chest compressions during CPR is determinant for survival from OHCA. CPR and defibrillation can be successfully taught to laypeople, and the use of automated external defibrillators (AED) by the public may shorten the time to defibrillation. Survival from witnessed ventricular fibrillation (VF) decreases by 10–12% for every minute defibrillation is delayed, but when CPR is provided the decline in survival is only 3-4% per minute. 
The most influential factor explaining survival is the interaction between CPR and defibrillation administered in the first minutes from collapse. The chain of survival involves four links: early recognition, early bystander cardiopulmonary resuscitation (CPR), early defibrillation, and early advanced care. In the early 1990s, the American Heart Association (AHA) established the chain of survival to describe the sequence of actions for a successful resuscitation in the event of an out-of-hospital cardiac arrest (OHCA). Our objective is to present a thorough review of the field as the starting point for these late developments and to underline the open questions and future lines of research to be explored in the following years. Moreover, new strategies for fast rhythm analysis during ventilation pauses or high-specificity algorithms have been reported. 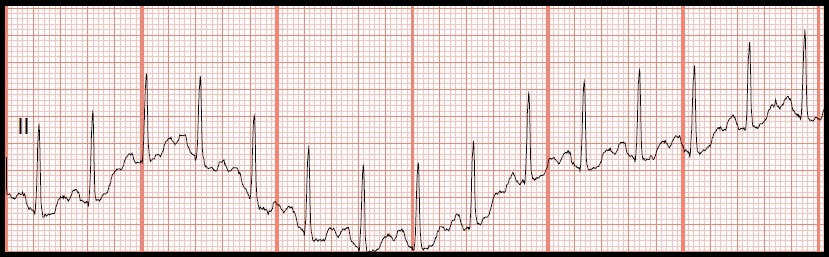
Recently, researchers have proposed a new methodology to measure this impact. In general, all the methods report low specificity values when tested on short ECG segments, but how to evaluate the real impact on CPR delivery of continuous rhythm analysis during CPR is still unknown. Most approaches are based either on adaptive filters to remove the CPR artifact or on robust algorithms which directly diagnose the corrupted ECG. In the last twenty years, research has been focused on designing methods for analysis of ECG during chest compressions. Unfortunately, interrupting CPR adversely affects survival. CPR must be interrupted for a reliable automated rhythm analysis because chest compressions induce artifacts in the ECG. Survival from out-of-hospital cardiac arrest depends largely on two factors: early cardiopulmonary resuscitation (CPR) and early defibrillation. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
